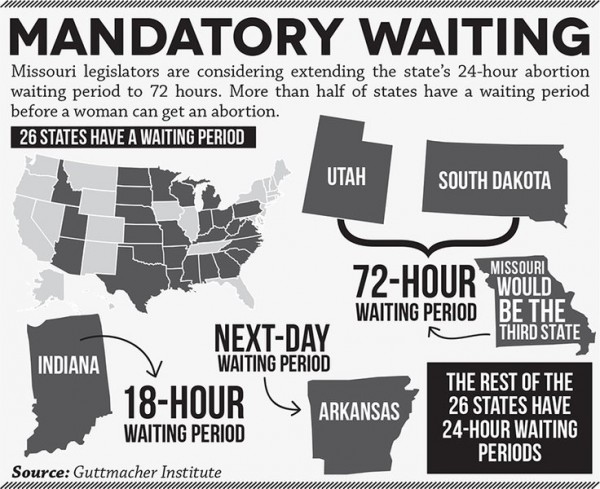
State laws limiting funding for abortion and requiring additional steps for women seeking abortion have been enacted for almost four decades, but more new restrictions were put in place between 2011 and 2013 than in the entire previous decade. At times, new enactments add new restrictions on top of older ones, such as lengthening the time periods in laws that require delays for women seeking abortions from 24 hours to 48 or 72 hours. Laws of this sort not only mandate that women seeking abortions must wait after hearing state-mandated information, they often require the information to be delivered in person rather than over the phone, so women have to make two visits. As of February 2016, 27 states mandated waiting periods, four of them with a 72 hour delay; and 13 states had rules that necessitated two visits.
Research on Utah’s 72-hour Waiting Period
Arguments rage about these laws. Advocates in support of them maintain that waiting periods are necessary to ensure that abortion providers will give women the time and opportunity to change their minds, while others argue that the logistical difficulties caused by waiting periods and two-visit requirements may prevent women from having abortions they want. Who is right? So far, researchers have not developed sound evidence about women’s actual experiences with these laws.
To help address this research shortfall, we, along with colleagues, have studied Utah’s 72-hour waiting period law, which in 2012 became the first 72-hour mandate to go into effect. Our study recruited 500 women who came for the required first abortion information visit at four family planning facilities in the state. Women completed iPad surveys before receiving the state-mandated information and any abortion counseling the facility routinely provided. Three weeks later, the women completed telephone follow-up interviews.
Did Waiting Periods Change Minds?
Eight percent of women we studied reported changing their minds about having an abortion, but most of them had still been making up their minds at their first visit. Strictly speaking, just 2% of our respondents were sure of their decision when they first arrived to receive abortion information and then decided afterwards not have the abortion. This estimated 2% for whom “change of mind” is a proper designation is similar to the proportion of abortion patients who, according to other studies, genuinely change their minds in settings where there are no waiting periods, or minimal ones. Statistical analyses confirm that women who are not conflicted about the abortion decision during their required information session are more likely to proceed than those who are highly conflicted. As has been found in multiple other studies, we found in our study that the vast majority of women had made their decision prior to arriving for the required abortion information visit and were not conflicted about their decision and most women (86%) proceeded to have abortions after the waiting period. In short, women do not seem to need special protection to make this decision.Delays and Two Visits Caused Hardships
Contrary to what some abortion rights advocates claim, we did not find that women were unable to have abortions because of the 72-hour waiting period and the need to make two visits. However, these cumbersome requirements did cause hardships for women, most of whom had already made a firm decision to obtain abortions before the information visit. Specific difficulties reported by these women included:
- A 10% increase in the cost of the abortion. For women whose average household income is $22,000 per year and who live in a state that does not allow Medicaid funding for abortion, this increase is not negligible.
- Waiting not just for 72 hours, but for an average of 8 days, more than a week, between the information visit and the abortion appointment. For women at an early stage and without pregnancy symptoms, this extra wait caused little apparent trouble, except for prolonged nervousness and forced attention to a decision they were ready to implement. However, a small number of women worried that the prolonged wait would push them beyond the time period when medication abortion was an option and lead them to incur extra costs due to being pushed into the second trimester. In one case, the mandated delay pushed a woman past her personal comfort point for proceeding to an abortion; and in another instance the waiting period pushed a woman beyond her facility’s gestational limit for abortion and so she did not have an abortion.
- Having to tell other people they were seeking an abortion. In order to arrange for the two mandated visits, six percent of women reported that they had to tell one or more people that they were seeking abortions – including bosses and coworkers, and men involved in the pregnancies, family members, friends, or child care providers.
Results and Implications
Overall, Utah’s 72-hour waiting period and two-visit requirement did not prevent women who had required information visits initial visits from proceeding to having abortions. But the legally required delays did burden women with extra financial costs and logistical hassles and caused them to dwell on decisions they had already made. Legally required delays made some women worry they would not be able to have the type of abortion they preferred and caused one to remain pregnant beyond her facility’s gestational limit for providing an abortion.Our study makes it clear that laws mandating waiting periods and two visits are blunt instruments that impose unnecessary difficulties on many women seeking abortions. Only a few women are truly conflicted about abortion decisions, and it seems more appropriate to use individualized patient education and counseling to assist them. In fact, most abortion facilities already provide such personalized counseling, just as providers do in other areas of health care.
Read more in Sarah Roberts, David Turok, Elise Belusa, Sarah Combellick, Ushma Upadhyay “Utah’s 72-Hour Waiting Period for Abortion: Experiences among a Clinic-Based Sample of Women,” Perspectives on Sexual and Reproductive Health (2016).

 Research to Improve Policy: The Scholars Strategy Network seeks to improve public policy and strengthen democracy by organizing scholars working in America's colleges and universities. SSN's founding director is Theda Skocpol, Victor S. Thomas Professor of Government and Sociology at Harvard University.
Research to Improve Policy: The Scholars Strategy Network seeks to improve public policy and strengthen democracy by organizing scholars working in America's colleges and universities. SSN's founding director is Theda Skocpol, Victor S. Thomas Professor of Government and Sociology at Harvard University.