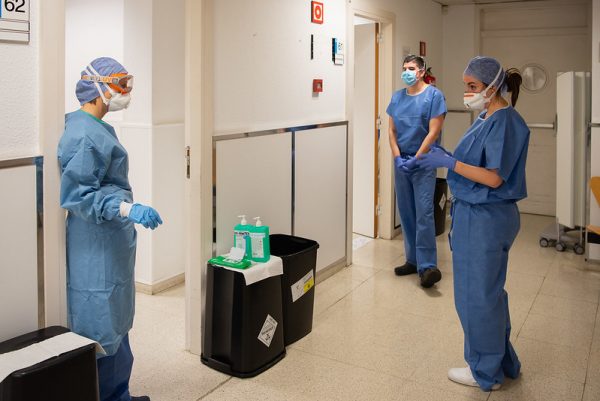
Medical sociologists Tania Jenkins (PhD, University of North Carolina-Chapel Hill) and Elaine Hernandez (PhD, MPH, Indiana University) pair up in this four-part series, COVID-19: Dispatches from Medical Sociology, to provide insight on how the current COVID-19 pandemic is changing the landscape of American healthcare. In the second segment, Jenkins and Hernandez discuss how COVID-19 is changing dynamics within healthcare professions.
- Social Inequities in Healthcare
- The Doctor Will “See” You Now
- Changing Dynamics within Healthcare Professions
- The Challenges Facing Medical Education
—
Changing Dynamics within Healthcare Professions
In addition to changing how healthcare is delivered, the COVID-19 pandemic is changing how healthcare professions are organized. While some workers are getting sidelined due to widespread furloughs (with roughly 43,000 healthcare jobs lost in March alone), others are being pressed into service in areas with more localized demand as the federal government urges states to expand their healthcare workforce. To that end, states have been temporarily loosening licensing regulations and suspending longstanding practice restrictions to expand the local health workforce.
For some advanced practice providers (APPs) — such as nurse practitioners (NPs) and physician assistants (PA) who generally require formal supervision by a physician — this has meant more autonomy and flexibility. In California, an executive order issued on April 14, 2020 expanded the number of nurse practitioners and physician assistants that a single physician can supervise from four to unlimited. Massachusetts and Virginia have waived the supervision requirement for advanced practice nurses with more than 2 years of experience. And, states like New York and Louisiana have temporarily suspended all supervision requirements for APPs, allowing them to practice as autonomous clinicians during the crisis.
These changes seem unremarkable in light of current crisis, but they stand in stark contrast to longstanding efforts from the American Medical Association (AMA) to maintain the status quo, with medical doctors (MD) at the top of the hierarchy of health care professionals. In 2019 alone, the AMA blocked “inappropriate scope expansions of nonphysicians,” more than 50 times at the state-level. Blocking these expansions ensured that APPs remained formally subordinated to MDs. Desperate times, and the need for more health care providers, has led to major shifts, though, at least in certain states — in other states, including California, medical associations successfully lobbied to maintain most of the practice restrictions against APPs, despite strong advocacy efforts on behalf of NPs and PAs.

It is unusual for federal and state government leaders to assert themselves so directly. Physicians have enjoyed a legal monopoly over medical care for nearly a century. Could these temporary changes pave the way for more permanent changes once the pandemic subsides? If NPs and PAs are able to practice safely without the usual restrictions during times of crisis, might they be able to continue doing so thereafter? Or will we return to the previous status quo?
We are not only observing major changes to the usual hierarchy between medical professionals, we are observing challenges to the usual social order within the medical profession. State governors have recently begun to ease longtime licensure restrictions against international medical graduates, allowing previously unauthorized physicians to practice during the crisis. New York, for example, announced last month that it would allow unlicensed graduates of foreign medical schools with at least a year of residency training to practice temporarily, while other states like New Jersey and Nevada have become begun to issue temporary licenses to physicians who are licensed and/or have trained in other countries than the United States (normally, international medical graduates are required to complete some amount of American training in order to be eligible for licensure).
The U.S. government has a long history of carefully titrating, or measuring and regulating, the influx of international medical graduates, variously ramping up or tightening supply depending on demand. Doing so results in a restricted number of U.S.-trained MDs filling spots in top specialties and hospitals, while lower-status international medical graduates fill less desirable jobs.
But with new policies opening the door to ever more foreign doctors, these hierarchies may start to shift. One of the myths that help sustain these status hierarchies is that international medical graduates are not as qualified as MDs trained in the United States, even though studies have found that patients treated by international graduates have equal or better health outcomes than those of U.S. physicians. Given the benefits to the healthcare system offered by these international medical graduates during the pandemic, should we consider more permanent paths to licensure thereafter?
The COVID-19 pandemic raises several unanswered questions for health professions as they continue to grapple with how to provide care in these times of crisis. The long-term impact of these policy changes on the healthcare professional landscape remains to be seen.
For more on this topic, check out sociologist LaTonya Trotter’s brand new book about nurse practitioners, More Than Medicine: Nurse Practitioners and the Problems They Solve for Patients, Health Care Organizations, and the State.
Stay tuned for our final installment on medical education.
